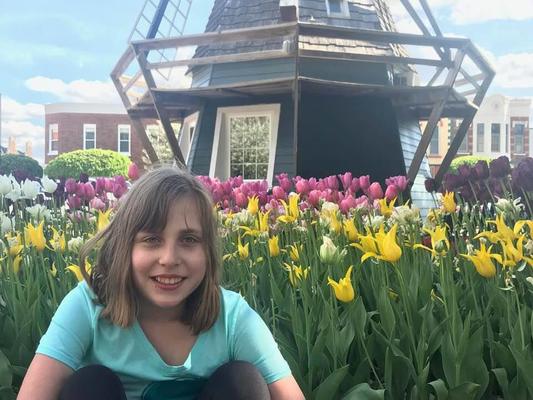Iowa girl thrives after ice-storm birth

By many accounts, 11-year-old Dorotea Orgovanyi is thriving: The Fairfield, Iowa, resident enjoys bowling, playing baseball, and zip-lining at summer camp. She likes to watch Friends, study math, and eat breadsticks at Olive Garden. She can twirl in one spot until onlookers feel queasy.
But her parents, Gabor and Janel, know better. They say if it hadn’t been for a pair of University of Iowa neonatologists, Dorotea—or Tea (“Tay-ah”), as her parents call her—likely wouldn’t be alive today.
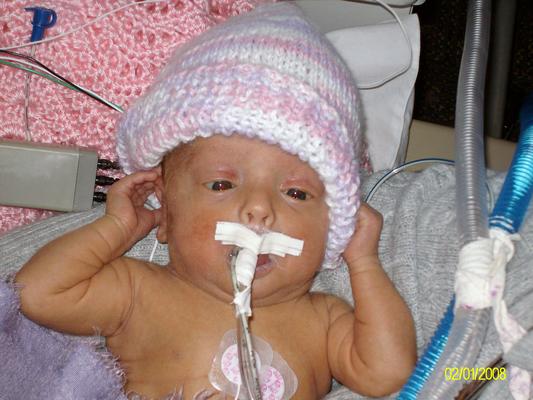
The night before Tea was born in December 2007, Janel experienced sharp pains in her abdomen. She was just 26 weeks pregnant, and having lost a baby in utero the year before, she took no chances and went to the county hospital in nearby Mount Pleasant. Tea was born the next morning, weighing just over a pound and a half.
John Dagle was still in bed when his phone rang. It was a fellow neonatologist at University of Iowa Stead Family Children’s Hospital. There was a baby girl some 50 miles away who needed their help. The staff at the local hospital was not equipped to deliver preemie care, and an ice storm was bearing down on eastern Iowa, grounding all emergency transportation services. Would Dagle join him in his SUV to drive down to Henry County and start treatment?
Dagle didn’t hesitate. He knew how critical the first few hours of life were for premature babies. Every organ was at risk for failure. Nothing could be taken for granted. He jumped into the car of now-retired Michael Acarregui, who had stuffed a bag of medicine and emergency supplies in the backseat, and the two ventured out onto the slippery highway.
University of Iowa Stead Family Children’s Hospital is home to the state’s largest neonatal intensive care unit, providing care for an average of 900 babies and their families each year. Expertise in every pediatric specialty is available 24/7, and the survival rate of all babies cared for in the NICU is more than 95%, placing it among the best in the nation.
When they arrived, the UI doctors began administering critical care to Tea, giving her medicine to open her lungs. Since the hospital didn’t have a ventilator designed for a preemie, Dagle directed the hospital staff to adapt a breathing device meant for adults with sleep apnea so they could manually deliver a precise mix of oxygen and air to the infant’s fragile lungs. In the meantime, a Henry County ambulance driver stepped up and volunteered to take Tea to Iowa City, so hospital staff began retrofitting the vehicle with a radiant warmer to hold Tea and keep her temperature steady.
Dagle accompanied Tea on the ride to Iowa City, standing beside her and squeezing air into her lungs every few seconds. Acarregui followed in his vehicle.
“Conditions that day weren’t ideal, and we didn’t have all the equipment we needed,” says Dagle, UI professor of pediatrics, biochemistry, and epidemiology and co-director of the Iowa Statewide Perinatal Care Program. “But that’s not what you think about when someone’s life is at stake. You think, ‘There’s a baby I can help,’ and you just do it. And I’d do it again tomorrow.”
The combined effort of the hospital staff, the ambulance driver, and the UI doctors willing to risk their lives to save hers helped ensure that Tea not only survived but ultimately grew into the chatty, inquisitive 11-year-old she is today.
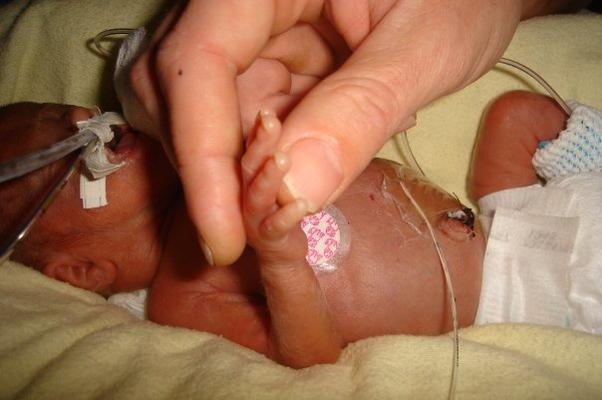
The early prognosis had not been good. Doctors initially told the Orgovanyis that their daughter may not walk or talk. Tea was only about the size of a Barbie doll, but her mom says she could tell that she was a fighter. And fight she did, through multiple complications, including a brain bleed, hydrocephalus, and heart surgery. Tea stayed at the UI hospital for three-and-a-half months after her birth, with Janel sleeping nearby in the Rossi Guest House and working from her laptop, and Gabor and Tea’s older sister, Tori, making trips to Iowa City as often as they could. The family has sought follow-up care for Tea at UI Stead Family Children’s Hospital ever since.
“Even though it’s an hour and a half away, we feel that the University of Iowa is close enough to get to in any type of emergency, and we know we’ll have the experts we need.”
“We know that if we lived anywhere else, the miracle that is Tea probably wouldn’t have happened,” says Janel. “We’ve used eight or 10 different university clinics due to complications from her birth, including cerebral palsy, epilepsy, and impaired vision. Over the years, we’ve had a few close calls and overnight stays at the university, and each time we feel as if we couldn’t be in a better place for our daughter. The UI Stead Family Children’s Hospital has been critical in getting the care she needs, whether in an emergency, follow-up care, or therapies, including those offered through the UI Center for Disabilities and Development.”
A care coordinator connected the family to local providers who work with the University of Iowa to coordinate Tea’s therapies and follow-up visits.
“The care at the University of Iowa has been wonderful,” Janel says. “We are forever thankful for each doctor, clinic, therapist, and nurse who has touched our lives and helped Tea become the wild child she is today. We couldn’t imagine a life without her in it.”

Dorotea, says Janel, truly reflects her name, which means “gift from god.”
“There’s no doubt that if we would have waited for an ambulance when the roads cleared, she would’ve died,” she says. “She didn’t have the medicine she needed to open her lungs. Breathing was definitely an issue, and the smaller hospital simply wasn’t equipped to help her.”
Dagle, who earned a PhD in biochemistry and a medical degree from Iowa in 1991 and has since been on the UI hospital staff, recently reunited with Tea for the first time and was thrilled to get a hug from her. He says he loves what he does as a neonatologist at the University of Iowa.
“It’s a good place to work and a great discipline. It’s not hard wanting to take care of kids,” he says. “When my first patient came back and said, ‘I’m going to high school,’ I thought that was really cool. Now, as I’ve gotten older, my first patients are going to college. They’re getting married, they’re having kids.”
“The cool part isn’t just having a baby live, it’s having a baby live and then have a great life.”